Hernia (Latin: hernia)— the exit of organs from the cavity they normally occupy through a normally existing or pathologically formed opening in anatomical structures while maintaining the integrity of the membranes covering them.
Clinical classification of hernias
By origin
- Acquired;
- Congenital.
It should be remembered that congenital hernias develop as a developmental defect, therefore they have their own etiological, topographic-anatomical and clinical features.
By the presence of complications
- Uncomplicated;
- Complicated (irreducibility, inflammation, phlegmon of the hernial sac, coprostasis, rupture of the viscera in the hernia, inflammation of the internal organs in the hernia and strangulation: elastic, fecal, mixed, retrograde (W-shaped) or parietal (Richter's hernia)).
By course
- Primary;
- Recurrent;
- Postoperative.
By reducibility
- Reducible (the contents of the hernial sac can easily be reduced into the abdominal cavity through the hernial orifice or can be reduced on its own)
- Irreducible (usually as a result of the development of adhesions, adhesions; the sudden development of irreducibility of a previously reducible hernia is a characteristic symptom of its strangulation)
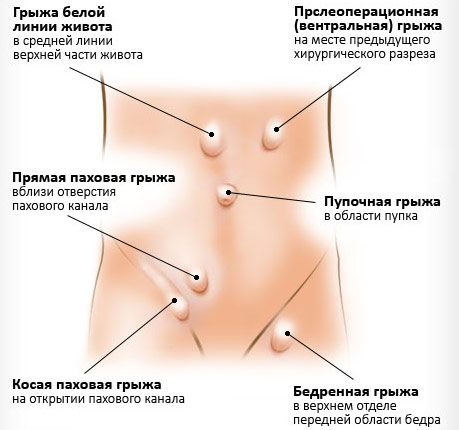
According to the place of occurrence, there are:
- inguinal;
- femoral;
- umbilical;
- postoperative hernias;
- hernias of the white line of the abdomen.
Diagnostics of hernias
In most cases, the diagnosis can be made based on a simple examination of the patient, when a protrusion is found in typical places, increasing with physical activity. In unclear cases, the surgeon can use additional research methods.
- Ultrasound of hernia allows you to determine the size of the hernial orifice, distinguish small irreducible hernias from soft tissue benign tumors of the subcutaneous fat (e.g., lipomas), enlarged lymph nodes in the inguinal region. It is especially useful for inguinal hernias.
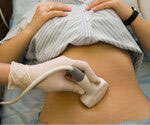
- Herniography is used in cases of unclear pain in the groin area (to exclude an externally invisible inguinal or femoral hernia), perineum (to exclude a perineal hernia) and in case of an inguinal hernia, if there is doubt about the presence of a hernia on the opposite side.
- Computer tomography allows you to clearly determine the nature and size of the abdominal wall defect.
In recent years, due to the widespread introduction of new technologies and the latest scientific achievements and the use of modern plastic and suture materials, the quality of herniotomy performed has significantly improved, as well as the number of relapses and postoperative complications has decreased.
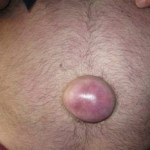
An umbilical hernia is a pathological protrusion of abdominal organs through the umbilical ring, which can disappear or significantly decrease in size when the body is in a horizontal position. This disease occurs in 6-10% of the adult population and is more often observed in women.
Symptoms
The severity of the symptoms of an umbilical hernia depends on many factors:
- its size;
- the presence of adhesions in the abdominal cavity;
- the presence or absence of strangulation of the hernial sac;
- the general condition of the patient.
The very first symptom of a hernia is the appearance of a small protrusion in the navel area. There may be no pain at first. At an early stage, you can even put the hernia back in place yourself, without a doctor. If adhesions appear, it will no longer be possible to put them back in place. The duration of the adhesion formation process is individual, so some people get used to putting the hernia back in place for years and continue living without going to the doctor, while others develop adhesions quite quickly.
Pain is not always present with an umbilical hernia in adults. It can appear during physical exertion, coughing, and standing in one place for a long time. Late stages can already be accompanied by nausea, vomiting, belching, constipation, and difficulty urinating.
Treatment
The only method of treating an umbilical hernia in adults is surgery. Surgery for umbilical hernia may be postponed in uncomplicated forms of the disease in pregnant women or in cases of concomitant diseases that aggravate the general condition of the patient (acute or exacerbated chronic diseases, pulmonary or heart failure, etc.).
Inguinal hernia
Classification
According to anatomical features, there are oblique, direct and combined inguinal hernias. Oblique inguinal hernias can be congenital or acquired.
Direct inguinal hernias are always acquired and are characterized by the protrusion of the peritoneum into the inguinal canal directly through the inguinal space, outside the spermatic cord. Combined inguinal hernias are complex formations consisting of several hernial sacs that do not communicate with each other and exit through different hernial openings.
There are also reducible inguinal hernias (which can appear and disappear) and irreducible ones, which cannot be eliminated independently due to the fusion of the hernial sac with the hernial contents. A sliding inguinal hernia is said to occur when the hernial sac is formed not only by the parietal peritoneum, but also by its visceral leaflet covering the sliding organ. A sliding inguinal hernia may include the wall of the urinary bladder, the cecum, the ovaries, the tubes, the uterus, etc.
If an inguinal hernia recurs after surgery, it is considered recurrent.
Based on the clinical course, uncomplicated and complicated inguinal hernias are distinguished.
- Non-strangulated inguinal hernias;
- Strangulated inguinal hernias.
With a strangulated inguinal hernia, the following clinical features are observed:
- sudden onset;
- irreducibility;
- sharp, gradually increasing pain;
- nausea, hiccups, repeated painful vomiting;
- stool and gas retention;
- severe condition of the patient;
- tension, soreness of the hernial protrusion.
The presence of these clinical symptoms is an indication for emergency surgery.
Symptoms of an inguinal hernia
- Volume formations appear at the site of the hernial protrusion. Its size can vary from a walnut to a chicken egg. The hernial protrusion can occur periodically and be easily retracted - spontaneously or by the patient (reducible hernia), or it can be present constantly (irreducible hernia).
- The patient begins to complain of periodic pain in the hernia area, which intensifies with physical exertion and can radiate to the scrotum, sacrum, lower back and lower abdomen. Over time, the pain becomes chronic and quite severe.
- A feeling of discomfort appears when walking.
Diagnostics
When examining patients with inguinal hernias, both inguinal regions are examined in a standing and lying position to detect (in unclear cases) asymmetry, even if barely noticeable, but giving some indication of the possible presence of a hernia.
Pasture of the superficial inguinal ring when inserting a finger and simultaneously tensing the abdominal wall (coughing) gives a "push symptom".
Examination of the superficial inguinal ring in women is much more difficult than in men, and is possible only with flabby skin and significant expansion of the superficial inguinal ring.
Treatment of inguinal hernia
Treatment of inguinal hernias includes surgical elimination of the defect in the abdominal wall. Closure of the hernial defect and restoration of the integrity of the abdominal wall can be performed using local tissues - aponeurosis (hernioplasty with own tissues) or a synthetic prosthesis (hernioplasty with installation of a mesh prosthesis). Today, tension-free methods of inguinal hernia plastic surgery using a mesh transplant are increasingly used in surgery. In this case, the hernial orifice is strengthened from the inside with a special polypropylene mesh, which subsequently serves as a frame for the growth of connective tissue and prevents the exit of internal organs. Tension-free hernioplasty reduces the likelihood of recurrence of inguinal hernia. Treatment of inguinal hernias can be performed laparoscopically.
Prognosis and prevention of inguinal hernias
In the long term, a relapse of an inguinal hernia is possible. Relapses develop especially often after tension hernioplasty. In other cases, the prognosis for work capacity and quality of life is favorable.
The tasks of inguinal hernia prevention include strengthening the abdominal wall muscles, combating constipation, quitting smoking, which leads to coughing, weight control, and wearing a bandage during pregnancy.
Hernias of the white line
A hernia of the white line of the abdomen manifests itself as a painful protrusion anywhere along the midline of the abdomen.
A hernia of the white line of the abdomen (also known as a preperitoneal lipoma) is a condition in which gaps form in the tendon fibers between the muscles along the midline of the abdomen, through which first fat and then abdominal organs come out.
Symptoms of a hernia of the white line of the abdomen:
- a painful protrusion of the midline of the abdomen, most often in the upper parts;
- pain in the upper abdominal regions, especially with straining and sudden movements;
- muscle separation (diastasis) along the midline of the abdomen;
- nausea, sometimes vomiting.
Depending on the location relative to the navel, the following hernias of the white line of the abdomen are distinguished:
- supraumbilical - above the navel;
- periumbilical - next to the umbilical ring;
- subumbilical - below the navel.
In some cases, hernias of the white line of the abdomen do not manifest themselves in any way and are discovered by accident.
Emergency care is required if the umbilical hernia is strangulated and the following symptoms appear:
- rapidly increasing abdominal pain;
- nausea, vomiting;
- if the hernia does not go back under gentle pressure while lying on your back;
- blood in the stool, no bowel movements or gas.
Prevention of a hernia of the white line of the abdomen:
- do not lift objects that are too heavy.
- training your abdominal muscles;
- wearing a bandage during pregnancy;
- eating right;
- using the correct technique for lifting weights.
Treatment of a hernia of the white line of the abdomen
A hernia can only be removed surgically in a hospital setting.
Types of surgery (hernioplasty):
- Local tissue plastic surgery - suturing of the defect of the white line of the abdomen with the elimination of possible diastasis of the rectus muscles. However, due to the weakness of the connective tissue and significant stress on the sutures after surgery, relapses (repeated hernia formation) occur in 20-40% of cases.
- Plastic surgery using synthetic prostheses - installation of a mesh to close the defect of the aponeurosis after eliminating diastasis of the rectus muscles in a hernia of the white line of the abdomen. The probability of relapse is very small. The operation is performed under anesthesia.
A feature of surgical treatment of hernias of the white line of the abdomen is that eliminating only the hernia is not enough. It is also necessary to eliminate diastasis of the rectus abdominis muscles.
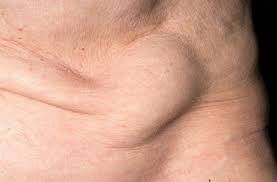
Spigelian hernia
Spigelian hernia is a lateral abdominal hernia that comes out through cracks in the aponeurosis of the abdominal wall along the lateral edge of the rectus abdominis muscle.
Specialists record this pathology with equal frequency in both sexes. In clinical practice, it is quite rare.
Diagnostics. The presence of a hernial protrusion and a defect in the aponeurosis along the line connecting the navel with the anterior superior iliac spine provides grounds for diagnosing a Spigelian hernia. The existing pain in the hernia area increases with physical exertion and decreases in a horizontal position. Due to the narrow hernial orifice, the Spigelian line hernia is often strangulated.
Treatment is surgical. To access the hernial sac and isolate it, various incisions are used: oblique, pararectal, transverse. The hernial sac is isolated and processed according to general rules. The stump of the hernial sac is immersed under the operant fascia. The edges of the muscles and aponeurosis are sutured.
Postoperative hernias
Postoperative hernia is a condition in which the abdominal organs (intestines, greater omentum) extend beyond the abdominal wall in the area of the scar formed after surgery.
Symptoms of a postoperative hernia
- painful bulge in the area of the postoperative scar;
- abdominal pain, especially when straining and making sudden movements;
- nausea, sometimes vomiting.
Course of a postoperative hernia
Postoperative hernias in the early stages are reducible and are not accompanied by pain. However, with sudden straining, falling, lifting weights, pain appears and the protrusion increases. As the hernia progresses, the pain intensifies, acquiring a cramping character. At the same time, intestinal sluggishness, constipation, flatulence, nausea develop; the activity of patients decreases sharply, fecal stagnation is periodically observed, accompanied by intoxication.
Causes of postoperative hernia
Postoperative hernia is a consequence of a previously performed surgical intervention. The determining causes for its development are:
- suppuration, inflammation of the surgical suture;
- increased physical activity after surgery;
- violation of the regimen of wearing a bandage in the postoperative period;
- insufficient recuperative forces and low immunity;
- obesity;
- severe cough, vomiting, constipation in the postoperative period;
- surgical errors made during the first operation.
Prevention of postoperative hernias
- wearing a bandage after abdominal surgery;
- proper nutrition;
- weight normalization;
- limiting physical activity in the postoperative period.
Treatment of postoperative hernia
The only way to get rid of a postoperative hernia is by surgery. Types of surgery (hernioplasty):
- Plastic surgery with local tissues - suturing the defect of the aponeurosis of the anterior abdominal wall. Local tissue plastic surgery is possible only if the defect is small - less than 5 cm. Local anesthesia is acceptable for small postoperative hernias, in other situations the surgery is performed under general anesthesia.
- Plastic surgery using synthetic prostheses - covering the aponeurosis defect in a postoperative hernia with a synthetic prosthesis. There are various methods, differing in the different placement of the mesh in the anatomical structures of the anterior abdominal wall. The probability of relapse is very low. The surgery is performed under general anesthesia.
