Platelet-rich plasma is a new highly effective method for treating diabetic ulcers.
Diabetic foot syndrome (diabetic foot) is a complex of anatomical and functional changes that develop against the background of diabetic neuropathy, micro- and macroangiopathy and osteoarthropathy. All these pathologies contribute to increased trauma and infection of the soft tissues of the foot, the development of a purulent-necrotic process and, in advanced cases, lead to amputation.
If you have had diabetes for several years, and especially if you have not controlled it well all this time, then there is a significant risk of developing serious complications.
There is a significant risk of developing serious complications of diabetes if:
- You have had diabetes for several years,
- If you do not control your diabetes well.
As you know, any wounds and injuries in patients with diabetes take a long time to heal. Even a small injury can fester and, if poorly cared for, gangrene can develop. This condition is difficult to cure and often ends in amputation. To avoid complications, study and carefully follow the rules for foot care, which are given below.
Symptoms, stages, forms
Symptoms and treatment methods depend on the form of the diabetic foot and the stage of development of the disease. The process is divided into 6 stages:
- 0 – risk group. There are no ulcers, but the feet are already deformed, pale and cold, calluses appear.
- Stage 1. Ulcers appear on the surface, but do not affect the deeper layers of the epidermis.
- Stage 2. The ulcer develops deep into the foot, affecting not only the skin, but also the muscles, tendons and tissue.
- Stage 3. The ulcer penetrates deep into the foot and reaches the bone.
- Stage 4. Blackness (gangrene) with clearly defined boundaries appears on the diabetic foot.
- Stage 5. The area of necrosis increases. Gangrene rises higher, capturing new foci. If left untreated, you can completely lose your leg.
Diabetic foot gangrene
Diabetic gangrene is the most severe form of diabetic foot. It develops if, against the background of severe circulatory disorders in the foot and lower leg, an infection occurs. This happens very quickly and very often leads to irreversible consequences.
The use of platelet-rich plasma at an early stage of ulcer treatment leads to its rapid healing.
Symptoms of diabetic foot
- Constant pain can be the result of a sprain, bruise, or uncomfortable shoes (shoes or socks "rub").
- Swelling of the foot is a sign of inflammation or infection, the result of wearing unsuitable shoes, or a consequence of venous congestion.
- The result of poor blood circulation in diabetics is:
- Pain in the legs or buttocks, increasing with walking and decreasing at rest;
- Hair loss from the shins and feet;
- The skin of the shins becomes dense and shiny;
- Local warmth is a sign of inflammation or infection of foot wounds.
- Any crack can develop into a serious pathology. Any callus or thickening of the skin is a sign of chronic foot injury.
- A fungal infection or ingrown toenail can develop into a more serious infection.
- Purulent discharge from a wound is a sign of a wound infection.
- Limping or difficulty walking may be signs of pathological changes in the joints, a serious infection, or improperly fitted shoes.
- A high body temperature (fever) in a diabetic patient with a foot wound may be a sign of a life-threatening infection.
- Spreading redness around the wound is a sign of a progressive infection.
- Numbness in the shins may be a sign of nerve damage (a complication of diabetes).
Prevention of diabetic foot
Prevention of "diabetic foot" is based on the treatment of diabetes as the underlying disease.
Maintaining vascular health also plays a major role in preventing complications of diabetes, which is achieved by controlling:
- Blood pressure level - no higher than 130/80 mm Hg,
- Blood cholesterol level - no higher than 4.5 mmol/l,
- And complete cessation of smoking.
Foot care for diabetes differs from the usual hygiene measures for people without diabetes. These rules take into account the fact that diabetes reduces the sensitivity of the feet, and any, even the smallest, damage can lead to serious consequences.
Foot gymnastics, massage and self-massage will help reduce pain and restore sensitivity.
Treatment of diabetic foot syndrome:
All complications of diabetes are potentially dangerous and require mandatory therapy. Treatment of diabetic foot should be comprehensive:
- Thorough treatment of the ulcer;
- Unloading the limb;
- Antibacterial therapy to suppress the infection;
- Compensation for diabetes;
- Giving up bad habits;
- Treatment of concomitant diseases that prevent ulcer healing;
- Restoration of blood flow.
Treatment of deep trophic ulcers:
Surgical treatment and the use of platelet-rich plasma, which gives a high chance of changing the outcome of the disease and leads to healing of ulcers.
If treatment is refused, as well as if the patient seeks help late, the situation worsens, which leads to the development of gangrene and further amputation.
Treatment of diabetic foot with platelet-rich plasma is becoming a more popular method, after many studies have proven its high efficiency. Using the patient's own blood makes the treatment safe and is not accompanied by an allergic reaction or infection. It is important that this treatment can be carried out on an outpatient basis. In the vast majority of cases, the result of treatment is the healing of ulcers.
Below are examples of diabetic foot treatment with platelet-rich plasma.
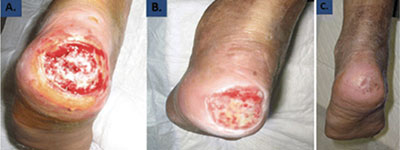
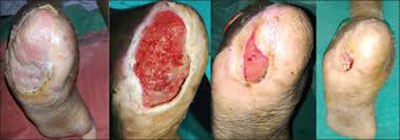
Pain and ulcers of the diabetic foot.
Diabetic foot is a common complication of poorly controlled diabetes mellitus, which develops as a result of skin injury, most often in the area of the big toes and heels.
Diabetic foot and pain can occur in all patients with diabetes, but good care and prevention can help prevent these complications from developing.
All patients with diabetes should consult a specialist if they experience discomfort, pain, or a wound in the foot.
Symptoms and diagnosis
One of the first signs of diabetic foot is the appearance of discharge from the foot. The most noticeable when examining the foot is the blackness (gangrene) surrounding the ulcers. This is a sign of skin necrosis due to lack of blood circulation. In addition, there is a foul-smelling discharge, pain, and numbness.
During the examination, your doctor will identify the severity of the situation on the following scale:
- 0 - no ulcer, some alarming changes in the foot;
- 1 - there is an ulcer without infection;
- 2 - a deep ulcer, joints and tendons are visible underneath.
- 3 - a large deep ulcer with signs of infection.
Causes of diabetic foot
- Poor blood circulation. Insufficient circulation leads to impaired blood supply to the feet, which complicates the healing of ulcers.
- Very high blood sugar.
- Neurological disorders can lead to persistent disorders and even loss of sensitivity.
- Damage to the skin of the foot.
Diabetic foot is a significant medical and socio-economic problem, which often ends in amputation.
Treatment of diabetic foot with platelet-rich plasma is becoming a more popular method after many studies have proven its high effectiveness. Using the patient's own blood makes the treatment safe and is not accompanied by an allergic reaction or infection. Importantly, this treatment can be carried out on an outpatient basis. In the vast majority of cases, the result of treatment is healing of ulcers.
